Podcast Episode #61: Postpartum Wellness

Dr. Erica of Root Functional Medicine gives moms some tips about staying healthy through pregnancy and into the postpartum period. We also talk about her upcoming Postpartum Wellness class on March 7. You can listen to this complete podcast episode on iTunes or SoundCloud. This podcast episode is sponsored by LifeFuel, providing healthy meal delivery […]
How ZENBands Became a Part of Pregnancy

Gold Coast Doulas is pleased to announce a guest blog by Dr. Erin Stair on her headbands that are perfect for listening to HypnoBirthing scripts or childbirth playlists. I use them for listening to podcasts like “Ask the Doulas” with Gold Coast Doulas on Soundcloud and Itunes. Erin is the creator of ZENBands, ZENTones, author […]
Podcast Episode #60: A Naturopath’s Perspective on Pregnancy and Depression

Doctor Janna Hibler, ND talks to Alyssa and Kristin about how a naturopathic doctor treats pregnant and postpartum women, body and mind. You can listen to this complete podcast episode on iTunes and SoundCloud. Alyssa: Hello, welcome to Ask the Doulas podcast. I am Alyssa Veneklase, co-owner of Gold Coast Doulas, and I am here […]
Healthy Prenatal Strategies for Pregnant Women

During pregnancy, the best health strategies are often those that can be incorporated into one’s everyday life. As a woman’s size increases and her mobility decreases, the ability to engage in physical activity gradually diminishes, which places a greater emphasis on other health habits that can help her maintain a healthy pregnancy weight and engage […]
Podcast Episode #38: Amber’s HypnoBirthing Story

We love hearing birth stories, especially from our clients. Listen as Amber tells us her birth story and how HypnoBirthing helped both her and her husband through 23 hours of labor. You can listen to this complete podcast on iTunes or SoundCloud. You can sign up for our HypnoBirthing classes here! Alyssa: Hello! Welcome […]
5 Research-Backed Strategies to Reduce Your Risk of Preeclampsia

If you’ve done any reading on preeclampsia, we’re probably in agreement that it’s a diagnosis that no woman wants to get. Preeclampsia is a pregnancy complication that affects up to 10% of expecting mamas. It involves high protein levels in the urine and swelling (edema) in addition to high blood pressure. Ultimately, these symptoms can […]
Podcast Episode #31: Rise Wellness Chiropractic

Dr. Annie and Dr. Rachel of Rise Wellness Chiropractic in Grand Rapids talk about their approach to helping mothers and babies, as well as how and why they decided to start their own practice. You can listen to the podcast on iTunes or SoundCloud. Hello, and welcome to another episode of Ask the Doulas. […]
HypnoBirthing – Brianna & Ben’s Story

A huge thank-you to our HypnoBirthing student for taking the time to share her beautiful birth story with us! We hope you love this as much as we do! My husband Ben and I decided to take a HypnoBirthing class because we had a goal to have a natural birth and because we didn’t think the hospital […]
Podcast Episode #22: How to get Dad on board with Hiring a Doula

On this episode of Ask the Doulas, Alyssa talks with Amber and Ashton about getting your husband or partner on board with hiring a doula. You can listen to this complete podcast on iTunes or Soundcloud. Alyssa: Hi, welcome to another episode of Ask the Doulas. I am Alyssa Veneklase, co-owner and postpartum doula, […]
Podcast Episode #12: Fertility Struggles

In this podcast episode, we talk with Lisa about her struggles with fertility and about the birth of her son, Ethan, who was conceived via IVF. This podcast is available to listen to on iTunes and Soundcloud. Alyssa: Hi, welcome to another episode of Ask the Doulas! I am Alyssa, co-owner of Gold Coast and post-partum […]
Podcast Episode #6: Dispelling The Goddess Myth

In this episode of Ask the Doulas, Alyssa and Ashley talk about The Goddess Myth and how it affects your birthing experience. You can listen to this complete podcast on iTunes. Alyssa: Hi, welcome to Ask the Doulas with Gold Coast Doulas. I am Alyssa, co-owner and postpartum doula, and today we have Ashley Forton […]
Podcast Episode #2: Having Kids Later in Life – Kristin’s Birth Journey

In this episode of Ask the Doulas, Kristin shares about her birth experiences and how she started the journey to become a birth doula. You can listen to this complete podcast on iTunes. Alyssa: Welcome to another episode of Ask the Doulas with Gold Coast Doulas. I am Alyssa, co-owner and postpartum doula, and […]
Make Your Hospital Room Feel Like Home

Today’s blog comes from one of our past birth doulas, Courtney Garvelink. Her experience with birth clients, as well as being a licensed massage therapist and previous HypnoBirthing instructor, makes her an expert on comfort measures in the delivery room. See what she has to say about making your hospital birth feel more like home. […]
Chiropractic Prenatal Care
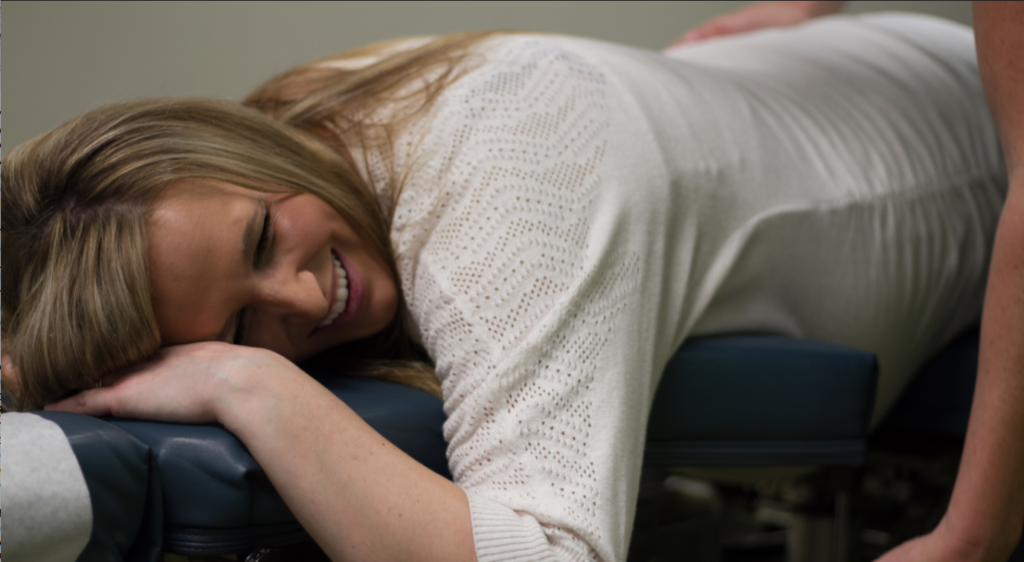
Yes, you read that right! If you just raised an eyebrow with a bit of confusion, you are not alone. Most people think Chiropractic care is mostly for neck pain, back pain, and maybe headaches. For most of my patients, that’s true. However, after we resolve their pain, some amazing things start happening. Some people […]
Meet our new birth doula, Angel!

1) What did you do before you became a doula? I have been a stay at home mom for the past (almost) four years. Before that I worked as a medical assistant in a few different areas, end of life care and a neurosurgeons office. 2) What inspired you to become a doula? I was […]
Healthy Fats for a Nourished Body & Baby

We are happy to have Sam Kalawart, Certified Health Coach, as a guest blogger today! Check out what she has to say about healthy fats. Pregnancy is a beautiful and exciting time in a woman’s life. During these 9 months, your body is working in over drive to ensure your unborn baby is developing as […]
Why Take a Breastfeeding Class?

Why Take a Breastfeeding Class? We are pleased to present a guest blog by Shira Johnson, IBCLC . Breastfeeding is natural, right? Well, yes… But it doesn’t always come naturally! Just like parents educate themselves about pregnancy and birth, it’s valuable to have basic knowledge about breastfeeding before baby arrives (we don’t read up on […]
12 Things To Do When You Are Overdue

It can be a struggle to get through the in-between time. Here are some things that West Michigan women can do in the final days of pregnancy. Please note–I did not contact businesses listed below in advance of this post. Here are 12 Things To Do When You Are Overdue: 1) Grab a smoothie or […]
Riding the Waves

Gold Coast Doulas is excited to feature a guest blog from Lauren Rauseo. Lauren is mom to Dylan, Liv and Fiona. She works part-time as a graphic designer is working to become a postpartum doula as well. Her favorite things are coffee, manicures, wine, yoga, and family dance parties in her living room. Now that […]
Is Your Pregnancy Missing Craniosacral Therapy
Gold Coast Doulas asked Kelly Marie O’Brien Pahman to guest blog on the topic of craniosacral therapy. Kelly opened St. Brigid’s Holistic Labor Care in 2009 where she works as a Holistic Doula and in 2014 she added St. Brigid’s Craniosacral Center in order to support clients and their families with Craniosacral therapy. She has […]


