How to raise perfectly imperfect kids with Lisa Sugarman: Podcast Episode #152

Lisa Sugarman, author of How To Raise Perfectly Imperfect Kids, discusses positive parenting and balance with Kristin. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about topics […]
Intentional Motherhood with Monique Russell: Podcast Episode #152

Kristin and Monique, author of Intentional Motherhood: Who Said It Would Be Easy?, discuss her book and share tips to connect with your children and communicate your needs with others to better enjoy this time of transition. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. […]
Ayurvedic Postpartum Healing with Ameya Duprey: Podcast Episode #151

Kristin and Ameya Duprey discuss the root causes of postpartum imbalances and how to heal them. Ameya is an Ayurvedic practitioner, postpartum doula and author. You can listen to this complete podcast episode on SoundCloud, iTunes, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to […]
Nursery Trends and Safety: Podcast Episode #150

Kristin chats with Naomi Coe, founder of Little Crown Interiors and author of Your Perfect Nursery about nursery trends and nursery safety. You can listen to this complete podcast episode wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about […]
The Ultimate Birth Experience: Podcast Episode #149

Kristin chats with Gail Janicola about what it means to have the ultimate birth experience. Gail is a birth expert, author of “The Ultimate Birth Experience,” and a mommy mentor. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a […]
Pregnancy After Loss: Podcast Episode #148

Gold Coast client Deb Kalsbeek shares her story of pregnancy after loss with Kristin. Deb also gives tips on how to best support grieving families. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to […]
Emergency: This Book Will Save Your Child’s Life – Podcast Episode #147

Kristin chats with Mark about how he came to write his book Emergency and why it’s important for expecting moms and dads to start thinking about safety issues about 8 weeks before birth! You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask […]
Ownership Change at Gold Coast Doulas

In 2015, when my daughter was 2 years old, I decided to leave my office job and become a postpartum doula. Kristin was one of the first doulas I met, and we actually took our postpartum trainings together. Little did we know that a year later she would call me to ask if I wanted […]
Happy with Baby: Podcast Episode #146

Kristin & Catherine, author of Happy with Baby, discuss the challenges of moving from partner to parent and how that can throw you for a loop. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk […]
Dancing with Fear: Podcast Episode #145

Kristin and Deb discuss how to prepare for birth when working through fear. Deb is the director of the Prenatal Yoga Center. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all […]
Sabrina, Founder of Osso Safe – Podcast Episode #144

Kristin chats with Sabrina of Osso Safe about preventing violence in a relationship and how OSSO safe can protect families. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the […]
Amber’s Postnatal Story: Podcast Episode #143

Kristin chats with Gold Coast client Amber Shaw about her postnatal recovery. She shares the challenges she faced and discusses how she advocated for her needs. You can listen to this complete podcast episode on iTunes or SoundCloud. You can also check out Amber’s birth story and her experience with the Becoming course. Welcome. […]
The Importance of Registering for Services: Podcast Episode #142
Kristin and Kaitlin McGreyes of Be Her Village discuss the importance of registering for services vs. things and her groundbreaking new gift registry platform. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts […]
Talking Formula Shortages with Kelly, IBCLC: Podcast Episode #141

Kristin and Kelly discuss the formula shortage and share resources to help families during this stressful time. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you get your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about topics […]
Benefits of Baby Massage: Podcast Episode #140

Kristin chats with Helen Thompson about the benefits of baby massage and the bonding that it provides for parents and the newborn. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all […]
Amanda Tice and The New Mom Code – podcast episode #139

Amanda Tice, model and author, talks about becoming a new mom. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you get your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about topics related to pregnancy, birth, postpartum, and […]
Meet our new birth doula, Lisa.

What did you do before you became a doula/consultant? I had a 20+ year career as an Occupational Therapist. Much of my career as a therapist, was at Mary Free Bed Hospital working in the wheelchair and custom seating department. Approximately 7 years ago, I completed my master’s degree and became an academic advisor. I […]
Harnessing the Power of Stem Cells Through Cord Blood Banking

Stem cells are special human cells that have the potential to become many different types of cells, such as brain cells, muscles cells, and more. These cells have the potential to treat, or even sometimes reverse diseases that have left patients of the past without effective options. Umbilical cord blood banking provides potential treatments for […]
Juliet’s Personal Preeclampsia Story: Podcast Episode #138

Juliet Meyer shares her personal preeclampsia story with Kristin that led to her work with the Preeclampsia Foundation. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you get your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about […]
Elizabeth King, Fertility Coach: Podcast Episode #137

Elizabeth King, Fertility Coach, shares helpful tips and resources for those who are struggling with conception and loss. You can listen to this complete podcast on iTunes, SoundCloud, or wherever you get your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about topics […]
Newborn Sleep – What New Parents Should Expect
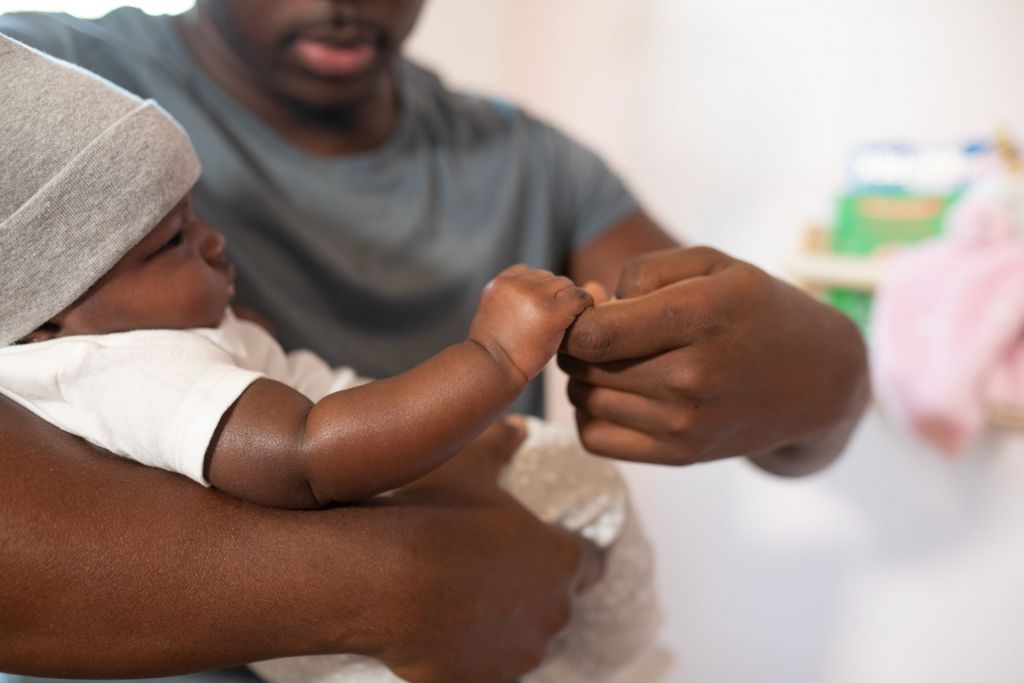
New parents often have unrealistic expectations about sleep when they bring a baby home. Some parents think they will get to sleep a lot because a newborn sleeps a lot. I’ve heard other parents say they don’t think they will get any sleep for weeks or months. I’m here to tell you that neither of […]
Amber’s VBAC Story: Podcast Episode #136

Kristin chats with Gold Coast client Amber Shaw about her VBAC birth story and the preparation she had for her birth. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over […]
Gold Coast Doulas is Expanding Our Reach!

We have been listening to our clients and trusted health practitioners, and we are expanding our day and overnight postpartum and sleep consulting services to Northern Michigan and Southwest Michigan starting in April of 2022. Michigan postpartum doula services and support will expand along the Gold Coast of Michigan, covering 300 miles of the western […]
Meet our new postpartum doula, Kristin M.

What did you do before you became a doula? Before I became a doula I worked in child care. I was a babysitter/ day care provider/ nanny for 20 years. I also am currently a preschool teacher. I have loved kids my whole life, and absolutely love working with them. What inspired you to become […]


