Meet our new postpartum doula, Jamie!

We are excited to have Jamie join our team. As a yoga instructor, she brings a sense of calm and balance to a room that immediately sets you at ease. Let’s learn more about her! What did you do before you became a doula? I spent a glorious taco-and-sun infused 6-years in Austin, Texas, doing […]
Megan’s Sleep Story: Podcast Episode #80

Megan Kretz, one of Alyssa’s sleep clients, tells us about her sleep training journey with her daughter at 9 months and again at 19 months. She says that as a working mom, it meant spending a little less time with her daughter, but that it was all worth it because the quality of the time […]
Supporting a Postpartum Mother: Podcast Episode #79

Elsa Lockman, LMSW of Mindful Counseling talks to us today about how partners, family members, and other caregivers can support a mother during those critical postpartum weeks to ensure she seeks help if needed. How do you approach a new mother and what are her best options for care? You can listen to this complete […]
Meet our new doula, Jen!

Meet Jen Serba, our newest postpartum doula. She filled out our standard Q&A so let’s get to know her a little better! 1) What did you do before you became a doula? I began my medical career 17 years ago when I became a Medical Assistant (MA) fresh out of high school. I was […]
Your Trusted Birth Team

We all know that becoming a parent is difficult, but most first time parents don’t really have a full understanding of how hard it will be until they’re in the midst of it. They may encounter fertility struggles or miscarriages; they realize that planning during pregnancy takes a lot of work; they have to find […]
Podcast Episode #68: Overnight Doula Support

Many of our clients and listeners don’t fully understand what overnight doula support looks like. Kristin and Alyssa, both Certified Postpartum Doulas, discuss the kinds of support their clients look for and how their team of doulas support families in their homes. You can listen to this complete podcast on iTunes or SoundCloud. You can […]
Podcast Episode #57: Sleep Consultations

Today we talk to Co-Owner of Gold Coast Doulas, Alyssa Veneklase, about sleep consultations. She talks about some common misconceptions and why her consultations are different. She says each sleep plan is unique and based on the individual family’s goals. Who knew you could still breastfeed and co-sleep if you want, all while getting […]
Podcast Episode #56: Traveling Postpartum Doulas

Will a postpartum doula travel? Yes, at Gold Coast they do! Today we talk to Kelsey Dean, a Certified Birth and Postpartum Doula, about her experience in California and in Michigan traveling with families as a postpartum doula and what that looks like. You can listen to this complete podcast episode on iTunes or […]
Podcast Episode #55: What Sets Gold Coast Doulas Apart?

What sets Gold Coast Doulas apart? Today Dr. Rachel of Rise Wellness asks us why she should refer her clients to us. She already knows she loves us, but why should everyone else? You can listen to this complete podcast on iTunes or SoundCloud. Kristin: Welcome to Ask the Doulas with Gold Coast Doulas. […]
Podcast Episode #54: What to Pack in your Birth Bag

Today Alyssa and Kristin talk to Dr. Rachel of Rise Wellness about what she packed in her birth bag. It’s one of the most common questions we are asked by birth clients. Find out what to bring and what you can leave at home! You can listen to this complete podcast episode on iTunes […]
Podcast Episode #51: Carrie’s Birth and Postpartum Story
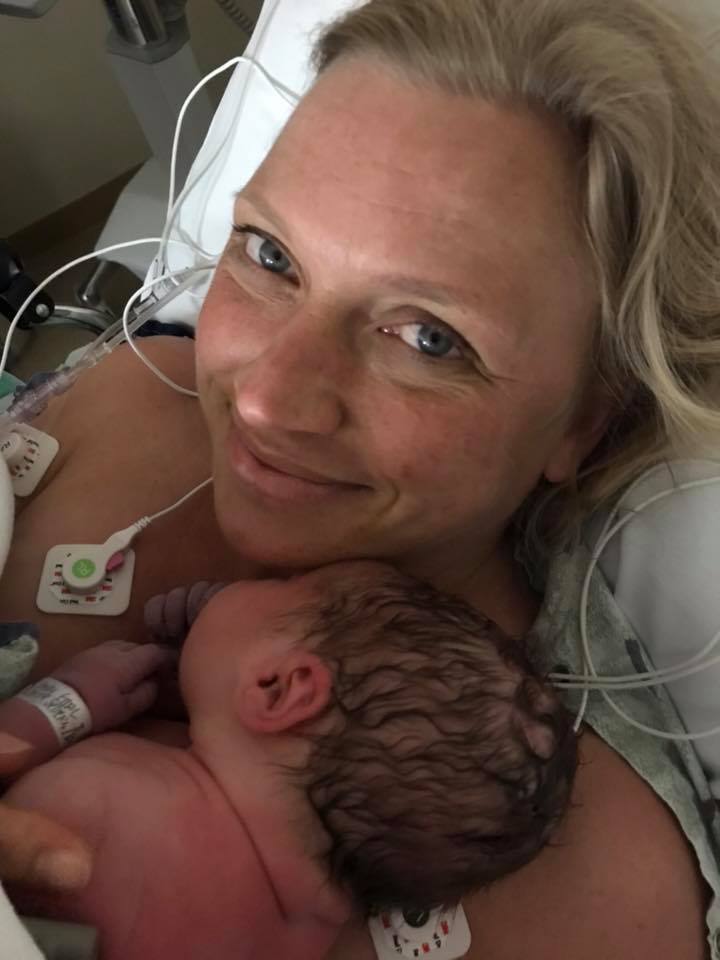
One of our clients describes her pregnancy, labor, and delivery and how having birth and postpartum doula support saved her sanity. You can listen to this complete podcast on iTunes or SoundCloud. Alyssa: Hello! Welcome to another episode of Ask the Doulas. I am Alyssa, and I’m super excited to be talking to one […]
Podcast Episode #17: How to Find a Babysitter You Trust

On this episode of Ask the Doulas, Alyssa and Cindy talk about how to find a babysitter that you trust to watch your kids. You can listen to this entire podcast epidode on iTunes and Soundclound. Alyssa: Hi, welcome to another episode of Ask the Doulas. I am Alyssa, and I’m here with Cindy from […]
Meet Your Gold Coast Doulas – Ashley

1) What did you do before you became a doula? I have a bachelor’s degree in health sciences from GVSU. I have been a nanny, worked at an adult foster care home and currently work in the insurance industry.. 2) What inspired you to become a doula? When I was pregnant I had an incredible […]


