Healing Childhood Trauma in Early Parenting: Podcast Episode #246

Emily Cleghorn shares her personal story of overcoming trauma and discusses the importance of support during motherhood on the latest episode of Ask the Doulas. She also discusses navigating triggers and tantrums as you heal your childhood trauma in the midst of early parenting. Emily is the founder of Mindful Soul Wellness. Hello! This is […]
Craniosacral Therapy for Infants with Meaghan Beames: Podcast Episode #240

Kristin Revere talks with Meaghan Beames of MyBaby Craniosacral Podcast and Beames CST Training Centre. They discuss how craniosacral therapy can help babies cope with colic, latching issues, and growing pains that can make life with a newborn harder than it needs to be. Hello, hello! This is Kristin Revere with Ask […]
Tips for Supporting New Parents with Lizzie Williams: Podcast Episode #239

Tips for supporting your friends who just had a baby with former Gold Coast Doulas client, Lizzie Williams. Kristin and Lizzie chat about everything from creating an intentional baby registry to her top tips for supporting new parents in the latest episode of Ask the Doulas. Lizzie contributed to our new book, Supported: Your Guide to […]
Simple Healthy Habits for Busy Moms: Podcast Episode #237

Kristin Revere and Brianna Wilkerson of Mommy Me Time Community discuss the focus on prioritizing health and self-care during each season of motherhood. Brianna has quick tips for both new and seasoned moms to get more intentional time and nourishment. Hello, hello! This is Kristin Revere with Ask the Doulas, and I am thrilled to […]
Green Beginnings: Six Essential Tips for a Safe, Low EMF Nursery

Guest blog post by Rebecca Pickett of Bebcare Low EMF Emissions Baby Monitors Creating an eco-friendly, green nursery is more than just a trend; it’s a commitment to the health and well-being of the newest addition to your family. By choosing non-toxic, sustainable materials, you’re reducing your baby’s exposure to harmful chemicals or wireless emissions […]
Heidi McDowell of Mind Body Baby Collective: Podcast Episode #235

Kristin and Heidi discussed her yoga studio’s expansion, including child care and a co-working space. They also discussed Heidi’s contribution to the fitness section in our upcoming book release, Supported: Your Guide to Birth and Baby. Hello, hello! This is Kristin Revere with Ask the Doulas, and I am thrilled to bring back Heidi McDowell […]
Top 5 Toddler Behavior Questions Answered with Christine Brown of Bella Luna Family! Podcast Episode #233

Kristin Revere and Christine Brown address everything from handling tantrums to managing a child’s big feelings in the latest episode of Ask the Doulas. You can listen to this episode on your favorite podcast player. Hello, this is Kristin Revere with Ask the Doulas, and I am thrilled to chat with my friend Christine Brown […]
We Wrote A Book! Podcast Episode #228

Kristin Revere and Alyssa Veneklase chatted about their upcoming book “Supported: Your Guide to Birth and Baby.” Their book will be released on Mother’s Day. Look for it on Amazon and ask for it at your favorite bookstore. The e-book and audiobook will be available in early June. Hello! This is Kristin Revere, and […]
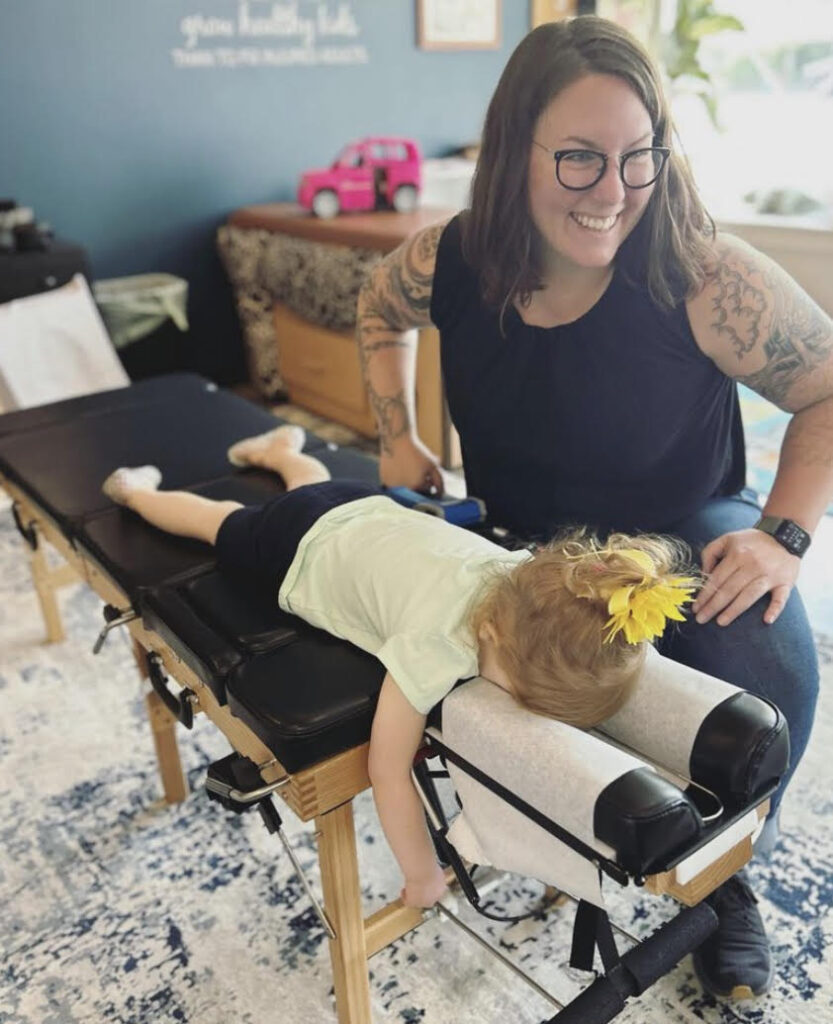
Webster Certified Chiropractic Care: Podcast Episode #226

Kristin Revere and Dr. Annie Bishop discuss how Webster Certified Chiropractic Care can be beneficial during pregnancy. They also discuss other options for prenatal and postnatal support. Hello, hello! This is Kristin Revere with Ask the Doulas, and I am excited to chat with my friend Dr. Annie Bishop of Rise Chiropractic Wellness. Welcome, Dr. […]
Did you forget something?

Gold Coast Doulas asked Heidi McDowell to guest blog on the topic of preparing your body for childbirth. Heidi is a yoga teacher at Mind, Body, Baby, a doula, a wife, and most importantly, a mama. Her goal is to create a community space for you that feels safe, supportive, and empowering. She holds certifications […]
Preparing for the New Parenting Role: Podcast Episode #224

Kristin and Danika discuss ways parents can prep for baby during pregnancy. They also touch on the role of social media in parenting. Hello, hello! This is Kristin with Ask the Doulas, and I am so excited to chat with Danika Sanchez today. She is the president and owner of Baby Steps Concierge Nursing. Welcome, […]
Caring for Newborns with Endira Davis: Podcast Episode #221

Kristin Revere chats with Endira Davis of Gold Coast Doulas about everything from infant swaddling to feeding in this fun episode on newborn care. They also discuss caring for twins and NICU babies. Hello, hello! This is Kristin Revere with Ask the Doulas, and I am so excited to chat with one of our own […]
Creative Movement: Podcast Episode #213

Kristin Revere chats about the importance of creative movement with Regina Lum of Little Feet Movement. Hello! This is Kristin with Ask the Doulas, and I am so excited to chat with Regina Lum today. Regina is a creative movement instructor, infant massage educator, and a self-proclaimed lay advocate. She owns Little Feet Movement for […]
How to Reawaken Your Imagination with Melissa Llarena: Podcast Episode #208

Kristin Revere chats with Melissa Llarena, author of Fertile Imagination: A Guide to Stretching Every Mom’s Superpower for Maximum Impact about how to reawaken your imagination! Ask The Doulas Podcast · How to Reawaken Your Imagination with Melissa Llarena This is Kristin with Ask the Doulas, and I am so excited to chat with Melissa […]
The Importance of Giving Back with Dr. Annie Bishop: Podcast Episode #202
Kristin Revere chats with Dr. Annie Bishop of Rise Wellness Chiropractic about the importance of giving back. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Welcome. You’re listening to Ask the Doulas, a podcast where we talk to experts from all over the country about topics […]
How to Prep for Infant Feeding with Victoria Facelli: Podcast Episode #201

Kristin Revere chats with Victoria Facelli IBCLC, author of Feed the Baby: An Inclusive Guide to Nursing, Bottle-Feeding and Everything in Between about the best ways to prep for infant feeding. Victoria has so many resources to help you! You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your […]
How to Create a Low Emissions Nursery for Your Baby

If you are expecting a baby or have a newborn at home, you may be wondering how to create a safe and healthy environment for them. One of the aspects that you may not have considered is the level of emissions in your baby’s nursery. Emissions are the invisible waves of energy that are emitted […]
Fair Play with Rachel Meakins: Podcast Episode #194

Kristin chats with Rachel Meakins from Zenbari about navigating household responsibilities using fair play. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Ask The Doulas Podcast · Navigating Household Responsibilities using Fair Play with Rachel Meakins Welcome. You’re listening to Ask the Doulas, a podcast where […]
The Impact of the Infant Microbiome on Health: Podcast Episode #192

Kristin Revere chats with Dr. Payal Adhikari of Infinant Health and the impact of infant microbiome on health. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Ask The Doulas Podcast · The Impact of Infant Microbiome on Health with Dr. Payal Adhikari of Infinant Health Welcome. […]
Finding Your Footing in Early Parenthood

Deb Porter, Owner of HOLD Hearing Out Life Drama, helps individuals improve their communication by teaching active listening skills resulting in positive outcomes. Deb also provides a safe, non-judgmental space so that those who use HOLD’s confidential listening service gain clarity and find relief from overwhelming situations. When Reality Doesn’t Match Expectations: You’ve dreamed of […]
Grandparents as Caregivers: Podcast Episode #186

Kristin chats with Kristin Morter of Gold Coast Doulas about the important role grandparents play as caregivers and how they should prepare themselves for taking care of a new little one. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Ask The Doulas Podcast · Grandparents as […]
Finding the Perfect Childcare Option: Podcast Episode #185

Kristin and Jaynie Fawley of Michigan Nanny Solutions chat about childcare options and finding the perfect nanny. You can listen to this complete podcast episode on iTunes, SoundCloud, or wherever you find your podcasts. Ask The Doulas Podcast · Finding the Perfect Childcare Option with Jaynie Fawley of Michigan Nanny Authority Welcome. You’re listening to […]
Breastfeeding and Infant Gut Health 101

Payal Adhikari, M.D. is a pediatrician and Clinical Implementation Director for Infinant Health. She grew up in the Chicago suburbs and lived in Singapore prior to settling in Chicago with her husband and two kids. She encourages her patients to have fun with parenting and believes in the power of the microbiome to influence positive […]
Informed Pregnancy with Dr. Berlin: Podcast Episode #178

Kristin chats with Dr. Berlin about the Informed Pregnancy Project. The Project aims to utilize multiple forms of media to compile and deliver unbiased information about pregnancy and childbirth to empower new and expectant parents to make informed choices regarding their pregnancy and parenting journey. You can listen to this complete podcast episode on iTunes, […]


