Rising Measles Cases: Podcast Episode #344

As measles cases rise again across the U.S., many parents are asking important questions: Is my child fully protected? What should I do if my family is exposed? How concerned should parents really be? In this episode of Ask the Doulas Podcast, Kristin sits down with Dr. Michael T. Myers Jr. to discuss what families need […]
Calm Crying and Boost Sleep with Dr. Harvey Karp: Podcast Episode #343

What if calming a crying baby and getting more sleep did not have to feel so overwhelming? In this episode, Kristin Revere sits down with Harvey Karp, renowned pediatrician, bestselling author of The Happiest Baby on the Block, and founder and CEO of Happiest Baby. Dr. Karp shares practical, science-backed strategies to help parents soothe fussy […]
Sleep Deprivation and Mood Disorders: Podcast Episode #342

Sleep deprivation is more than just part of new parenthood. It can have a serious impact on mental health during pregnancy and postpartum. In this episode of Ask the Doulas Podcast, we’re joined by Mariana Yancik of Gold Coast Doulas to explore the powerful connection between sleep deprivation and perinatal mood and anxiety disorders (PMADs). Mariana […]
Beyond The Discharge Papers: Podcast Episode #341

What happens after you leave the hospital with your newborn—and no real roadmap? In this episode, we dive into the reality that no discharge paper can truly prepare you for the postpartum experience. Kristin is joined by Ciara Lyons, MSN, RN, PHN, to explore the physical, emotional, and mental transitions that new parents face once […]
Budgeting for Birth and Baby: Podcast Episode #340

Planning for a baby isn’t just about choosing the perfect registry items—it’s about preparing financially for pregnancy, birth, and life with a newborn. In this solo episode of Ask the Doulas, Kristin Revere of Gold Coast Doulas breaks down what families really need to budget for (and what they don’t). From prenatal care and delivery […]
Sleep Solutions That Actually Work: Podcast Episode #339

Sleep struggles are one of the most common challenges new parents face – but with so much conflicting advice, how do you know what approach is right for your baby and your family? In this episode of Ask the Doulas, we’re joined by sleep consultant Mariana Yancik of Gold Coast Doulas to break down the differences […]
Daycare Sleep Made Simple: Podcast Episode #338

If you’re preparing your baby for daycare—or already navigating unpredictable naps—you are not alone. In this episode, we’re joined by certified pediatric sleep coach Allison Egidi, founder of Sleep and Wellness Coach, who has helped over 1,000 families improve their child’s sleep. We dive into how daycare environments impact sleep, why naps can look completely […]
The Rise of Birth Centers: Podcast Episode #337

In this episode of Ask the Doulas, we’re joined by Lauren McCullough, a labor and delivery nurse turned birth center strategist and founder behind multiple national initiatives transforming maternal health. Lauren shares the vision behind the National Birth Center Directory and the growing momentum of March for Midwives—two powerful efforts designed to increase access, visibility, […]
Dog Meets Baby: Podcast Episode #336

Bringing home a new baby is a major transition for the entire family, including your dog. In this episode, we sit down with Dominika Knossalla-Pado, certified dog trainer and founder of Dog Meets Baby, to talk about safely preparing your dog for life with a newborn. Dominika shares her personal journey into motherhood and how […]
Gentle Sleep Training with Mariana Yancik: Podcast Episode #335

Sleep struggles are one of the most common challenges new parents face—but with so much conflicting advice, how do you know what approach is right for your baby and your family? In this episode of Ask the Doulas, we’re joined by sleep consultant Mariana Yancik of Gold Coast Doulas to break down the differences between gentle […]
Pregnancy Brain Fog and Perinatal Wellness: Podcast Episode #334

Is “pregnancy brain” real—or is there more going on beneath the surface? In this episode, we’re joined by Becky Gleed of the Perinatal & Reproductive Wellness Group to unpack the very real experience of brain fog during pregnancy and postpartum . From forgetfulness and mental fatigue to the emotional load of motherhood, Becky shares what’s […]
Finding Your Doula on Social Media: Podcast Episode #333

In this episode of Ask the Doulas, we’re talking all about social media and doulas with Doula Darcy. Social media has become one of the most powerful ways for families to discover support during pregnancy, birth, and postpartum, but it can also feel overwhelming to navigate. Darcy shares practical tips for parents on how to […]
Sensitive Skin and Newborns: Podcast Episode #332

Sensitive skin and newborns often go hand in hand, leaving parents overwhelmed, exhausted, and unsure of what products are truly safe and effective. In this episode, we sit down with Andrea Faulkner Williams, co-founder of Tubby Todd Bath Co., to talk about navigating dryness, eczema, and reactive skin in babies. We dive into why newborn […]
Mom Groups and the Power of Community: Podcast Episode #331

Mom groups have been making headlines lately, and not always in a positive way. While stories about mom group drama and social tension can get attention, they don’t reflect what supportive communities are truly about. The right mom group can be a lifeline during pregnancy and postpartum, offering connection, encouragement, and practical support when families […]
Let’s Talk Baby Formula: Podcast Episode #330

Choosing a baby formula can feel overwhelming, especially in a world full of strong opinions and fear-based messaging. In this episode, I’m joined by Mallory Whitmore, known as The Formula Mom, to have an honest, judgment-free conversation about formula feeding. We break down the different types and formats of baby formula, how to read ingredient […]
The Value of a Baby Prep Class: Podcast Episode #329

In this episode of Ask the Doulas, host Kristin Revere is joined by Alyssa Veneklase, pediatric sleep consultant and co-host of the podcast, to talk all about Newborn Survival and why a baby prep class can be one of the most valuable tools for expecting parents. We break down what families actually need to know before bringing a newborn […]
What is a Sibling Doula? Podcast Episode #328
When families prepare for birth, so much focus is placed on supporting the birthing parent and partner. But what about older siblings? In this solo episode with Kristin Revere, co-host of Ask the Doulas and founder of Gold Coast Doulas, we explore the role of a sibling doula and why this often overlooked form of […]
Sleep Classes & Sleep Consulting: Podcast Episode #327

In this episode of Ask the Doulas, we sit down with Alyssa Veneklase, pediatric sleep consultant and co-host of Ask the Doulas, to break down the difference between taking an infant or toddler sleep class and working one-on-one with a sleep consultant. We explore what families can expect from each option, who benefits most from a class […]
Fertility After 35: Podcast Episode #326

In this episode of Ask the Doulas, host Kristin Revere sits down with Dr. Katie Wood, Doctor of Pharmacy and CEO of Happy Nourished Motherhood, to discuss advanced maternal age and egg quality. Dr. Wood shares what truly impacts egg health as we age, common myths around fertility after 35, and how nutrition, lifestyle, and mindset […]
What Does a Daytime Postpartum Doula Do? Podcast Episode #325

Ever wonder what a daytime postpartum doula actually does? From helping you rest and recover to supporting feeding, soothing, and household routines, this episode breaks down what a typical daytime shift looks like — and why it’s so valuable for new parents. Listen now on Ask the Doulas podcast to hear Kristin Revere, CEO of Gold Coast Doulas walk […]
Alternatives to Traditional Baby Showers: Podcast Episode #324

In this episode of Ask the Doulas, Kristin Revere of Gold Coast Doulas explores creative ways families and friends can celebrate pregnancy, honor expecting parents, and offer support without the typical party format. From meal trains and nesting parties to postpartum prep gatherings and intimate blessing ceremonies, we break down fresh ideas that focus on connection, […]
How Doulas Support Inductions: Podcast Episode #323
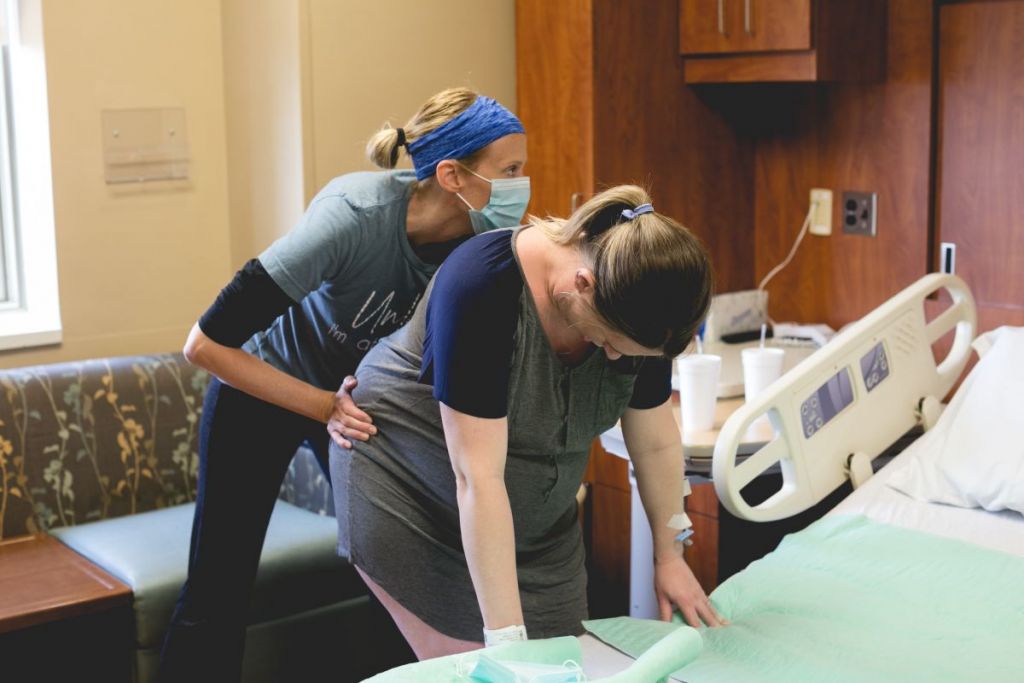
In this solo episode of Ask the Doulas, host Kristin Revere, founder and CEO of Gold Coast Doulas, explores how doulas can offer calm, confident support during labor inductions. Kristin breaks down what to expect when an induction is recommended, from the different medical methods to the emotional journey that often comes with it. She shares […]
Doula Business Structures Explained: Podcast Episode #322

In this solo episode of Ask the Doulas, Gold Coast Doulas founder Kristin Revere explores the different ways birth and postpartum doulas structure their businesses, including solo practices, partnerships, collectives, and agencies. This episode is a valuable resource for families who are deciding which model of care best fits their needs, as well as for […]
Doulas Don’t Replace Partners: Podcast Episode #321

In this solo episode of Ask the Doulas, Kristin Revere addresses one of the most common misconceptions about doula care — that hiring a doula might replace the partner during birth or postpartum. Whether you’re a partner wondering how a doula fits in or a parent curious about building your birth and postpartum team, this episode […]


