Why Babies Love Faces, Patterns, and Movement

Understanding the natural instincts behind newborn attention If you’ve ever held a newborn and noticed them staring intensely at your face—or at a bold pattern on a blanket—you’ve witnessed something remarkable. Even in the earliest weeks of life, babies are wired to notice specific things in their environment. Faces Movement High-contrast shapes These early visual […]
The Surprising Science of Newborn Vision

What Babies Actually See in Their First Months (and How Parents Can Support It) When a baby is born, we often assume they see the world the same way we do—just a smaller version of adult vision. But the truth is much more fascinating. Newborns enter the world with vision that is still rapidly developing, […]
The 4-Month Regression: What’s Happening & How to Survive It

Your baby was sleeping beautifully—maybe even giving you those glorious 4- to 5-hour stretches. You finally felt human again. And then, out of nowhere, everything falls apart. Suddenly, your once-great sleeper is waking every hour, fighting naps like it’s their job, and you’re wondering what on earth happened. This is the 4-month regression. Honestly, this […]
What Does a Daytime Postpartum Doula Do? Podcast Episode #325

Ever wonder what a daytime postpartum doula actually does? From helping you rest and recover to supporting feeding, soothing, and household routines, this episode breaks down what a typical daytime shift looks like — and why it’s so valuable for new parents. Listen now on Ask the Doulas podcast to hear Kristin Revere, CEO of Gold Coast Doulas walk […]
The Power Pumping Schedule to Increase Supply

Your milk supply feels like it’s not keeping up. But statistically, you’re not alone. Studies show that nearly 60% of new parents stop breastfeeding earlier than planned, with lactation and supply concerns being one of the main reasons. And you’re determined to boost your supply before making any big changes—we get it! The problem is, […]
What to Expect During Your Hospital Postpartum Stay: Podcast Episode #317

In this episode of the Ask the Doulas podcast, we’re joined by Kristin Morter, a Certified Elite Postpartum Doula and Certified Lactation Consultant, for a clear and reassuring look at what really happens during your hospital postpartum stay. Kristin walks us through the typical timeline from immediate recovery and newborn assessments to feeding support, rest, and those […]
Postpartum Traditions through an Ayurvedic Lens: Podcast Episode #314

In this enlightening episode of Ask the Doulas podcast, we explore postpartum traditions through an Ayurvedic lens with Christine Eck, Founder and Director of the Center for Sacred Window Studies. Christine shares why the sacred window—the first 42 days after birth—is such a vital time for healing, bonding, and transformation. We discuss how ancient Ayurvedic wisdom aligns beautifully with modern […]
Postpartum Night Sweats: Podcast Episode #312

Ever woken up drenched and wondering if you’ll ever sleep comfortably again? You’re not alone. In this candid episode of Ask the Doulas, we dive into the all-too-common struggle of postpartum night sweats, sharing our own experiences and giving some tips for relief. We’re joined by Jackie Hutson, founder of Piper & Mint, a brand redefining postpartum comfort with mint-infused, […]
The Grandparent’s Guide to Truly Helping After Baby Arrives

Congratulations—you’re about to become a grandparent! There’s something magical about watching your child step into parenthood themselves. Here’s the thing, though: the role of a grandparent has completely evolved. The old “let me know if you need anything” approach no longer works. New parents are exhausted and don’t even know what they need help […]
The Role of a Postpartum Doulas: Podcast Episode #308

Kristin Revere and LaVita Brown discuss the day in the life of a daytime and overnight doula. LaVita shares multiple examples of what her days look supporting families in West Michigan. Hello, hello! This is Kristin Revere with Ask the Doulas, and I’ve got a very special episode today, bringing on one of our […]
How a Night Nanny Can Help You Recover Faster Postpartum

The aftermath of bringing a baby into the world involves much more than figuring out your new family routine. You might also run into some roadblocks like sleep deprivation (because let’s face it, the word ‘sleep’ isn’t in a baby’s vocabulary), physical healing, and emotional adjustment. The thing is, all of this can be overwhelming […]
Teething Tips
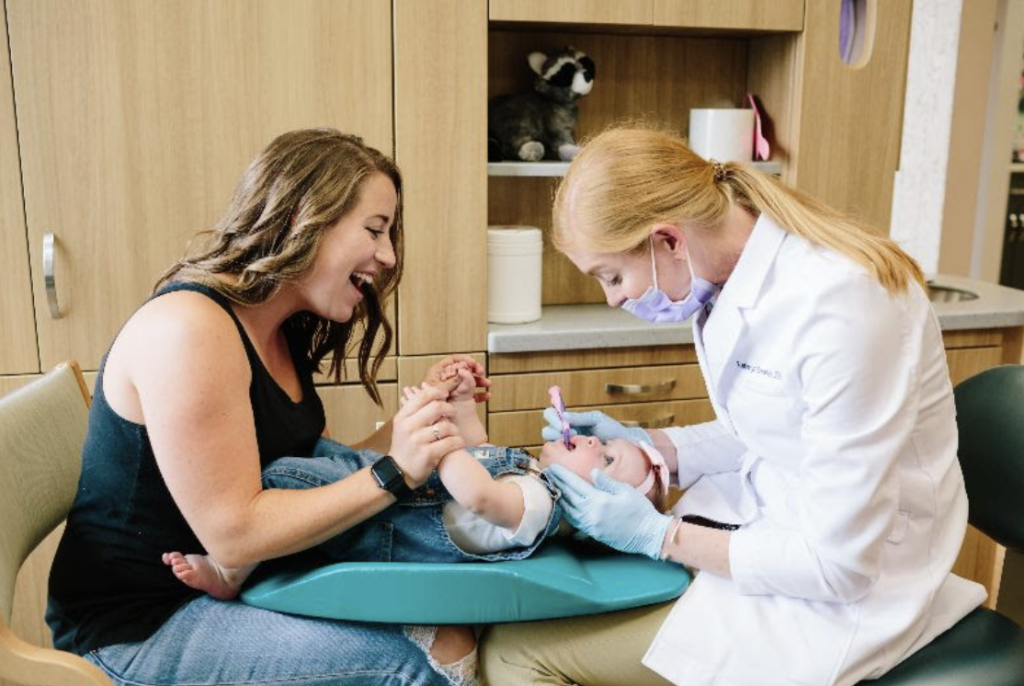
Written by Dr. Katie Swanson, Pediatric Dental Specialists of West Michigan As a pediatric dentist, one of my favorite roles is helping parents navigate their little ones’ teething symptoms. It can be a stressful time! Below are some truths, myths, and tips to help make the growing pains of teething easier on your baby or […]
Overnight Doula Cost: What You Can Expect to Pay

Most parents know that sleep deprivation naturally comes with the newborn territory. With late-night feedings, sleep regressions, unexpected fussiness, and never-ending schedule changes, the exhaustion is bound to hit—especially within the first few weeks. But, thankfully, that’s where overnight doulas step in to save the day… or night! Overnight doulas are trained professionals providing helpful […]
What Does a Night Nanny Do All Night?

To put it lightly, night nannies are lifesavers for new parents. There’s no question about it—they swoop in at the right moment when parents need extra help and give back those precious ZZZs that (if we’re being honest) are lacking at the moment. Because the reality is, losing sleep when you’re freshly postpartum can wreak […]
The Best Bottle Feeding Positions for Newborns

Honestly speaking, bottle feeding your newborn can be a learning curve. It’s one of those new parent duties that seems simple in theory but can get a little messy in those early days. (Insert acid reflux, sucking in too much air, tummy troubles, and tired arms) The good news? Many of these can be fixed […]
Wow, I’m honored to say the least!

When I first sat down to co-write “Supported: Your Guide to Birth and Baby,” I wanted to create something real. A guide that felt more like talking to a good friend than reading a health textbook. So we intentionally filled it with real-life experiences, evidence-based information, expert insights, and raw stories from both professionals and […]
Bottle-Feeding Pitfalls: Podcast Episode #296

Kristin Revere and Barbara Nelson, CLC discuss bottle-feeding pitfalls on the latest episode of Ask the Doulas Podcast. Barbara is a Pediatric Speech and Language Pathologist and Certified Lactation Counselor who specializes in infant feeding. She creates educational content to help parents feel confident in feeding their babies and recognize red flags early. She is […]
The 5-5-5 Rule: Postpartum Healing

To help freshly postpartum moms adjust and heal, a trending practice is becoming popular again—the 5-5-5 postpartum rule. This method encourages moms to rest and relax during the first 15 days at home with their baby. That means no cleaning sprees, no pressure to “bounce back”, and definitely no playing hostess. Just rest, recover, and […]
Travel Sleep Tips with Erin Junker: Podcast Episode #293

Kristin Revere and Erin Junker, CEO of the Happy Sleep Company, discuss everything from hotel stays to schedules on the latest episode of Ask the Doulas Podcast. Hello, hello! This is Kristin Revere with Ask the Doulas, and I am thrilled to chat with Erin Junker. Erin is a pediatric sleep consultant and owner of […]
Pacifier Safety with Lindsay DeOliveira: Podcast Episode #292

Kristin and Lindsay DeOliveira chat about how she came to start Soothe Beginnings after she struggled to find the perfect pacifier for her daughter. They also discussed her focus on safety and evidence-based design. Lindsay is also a baby registry consultant with Gold Coast Doulas. Hello, hello! This is Kristin with Ask the Doulas, […]
The Importance of Sharing Birth Stories: Podcast Episode #291

Kristin Revere and Dr. Elliot Berlin discuss the importance of reading or listening to birth stories and why it is valuable to share or record your own birth stories. Dr. Berlin hosts a narrative podcast on birth stories called “One Way or a Mother” as well as the “Informed Pregnancy Podcast”. Hello! This is […]
Mama Bear Survival: Podcast Episode #290

Kristin Revere and Emily Richett discuss Preparedness for Moms during pregnancy and early parenting in the latest episode of Ask the Doulas podcast. Emily is the author of “Mama Bear Survival: Raising Strong Families in an Uncertain World- A Guide to Preparedness, Resilience & Self-Reliance”. She is also the host of Mama Bear Survival […]
Roadmap to Raising Children: Podcast Episode #289

Kristin Revere and Dr. Karen Molano discuss the importance of pregnancy and the first five years of parenting. Dr. Karen Molano is a child psychologist and infant, family, and early childhood specialist. She utilizes her LumiTot Method to guide families through pregnancy and the first five years, providing them with a roadmap to raising children. […]
Harnessing Technology for Your Fourth Trimester: Podcast Episode #288

Kristin talks with Sarah Trott, founder of HelloGaia Parenting Copilot, about how technology helps parents simplify the overwhelming and find evidence-based scientific information to better prepare for the postpartum phase. Sarah is also the founder and host of the Fourth Trimester Podcast. Hello, hello! This is Kristin with Ask the Doulas, and I am […]


